Digestive Health & GI
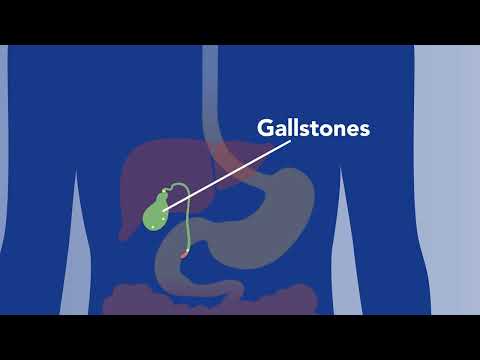
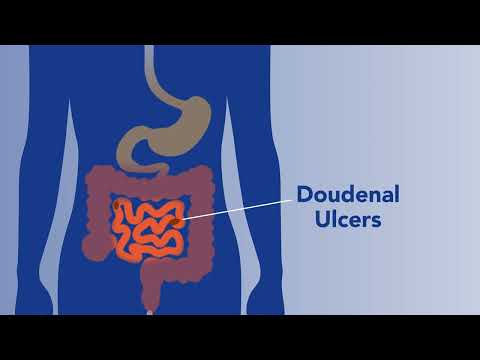
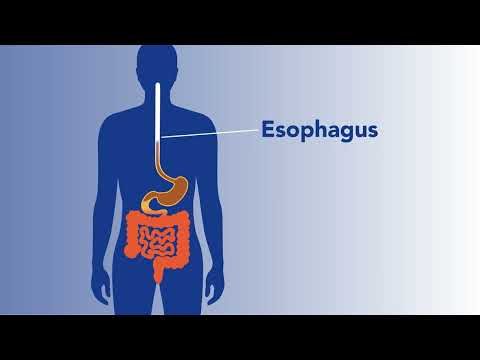
Your digestive system is responsible for breaking down food, absorbing nutrients and ridding your body of waste. The digestive system starts in your mouth and runs from your esophagus to your stomach to your intestines to your anus — i.e., your gastrointestinal, or GI, tract. Your liver, pancreas and gallbladder are also part of the digestive system. When one part stops working the way it’s supposed to, ripple effects often occur throughout the digestive system.
We are committed to collaborative, multidisciplinary care, which means you’ll work with a gastroenterologist, your primary care provider and other specialists, as necessary, to receive the most effective management.
Next Steps
Connect with a Gastroenterologist
Our specialists treat a full range of digestive diseases and disorders, offering the latest in advanced diagnostic, surgical, and nonsurgical options.
Learn about Colon Health
Is your colon healthy? Learn more about conditions, regular screenings, and treatments.
Hear From One of Our Doctors
Learn more about our digestive health risk assessment.
Your Digestive Health
Introduction – The Digestive System
Common Digestive Ailments
Diagnostic Procedures
Diagnosing Digestive Disorders
At Lake Cumberland Regional Hospital, our goal is to help patients find relief from the symptoms of digestive disorders so they can live a healthy, fulfilling life. Digestive disorders are complex and can affect the digestive system in a variety of ways, for a variety of reasons. In some cases, symptoms are subtle, resemble those of other conditions, or come and go over periods of time.
Our team uses a variety of tests and procedures to identify digestive disorders, including:
- Biopsy
- Blood tests
- Colonoscopy
- Lower GI series
- Stool analysis
- Upper GI series
- Video capsule endoscopy
Preventing Digestive Problems
Some digestive diseases and conditions have genetic components, and others may occur for unknown reasons. But many can be prevented or minimized with simple solutions, like changing your diet and exercise habits. Some of these changes include:
- You might be able to prevent heartburn, or acid reflux, by avoiding rich or highly acidic foods. But if that’s not enough, try eating smaller meals. Drink more water and save soda or alcohol for special occasions. Don’t eat close to bedtime. Elevating the head of your bed may also help.
- Exercise is important for maintaining your gastrointestinal and digestive health, especially as you age. Aim for at least two and half hours each week, and mix cardiovascular activity with muscle-strengthening routines.
- A healthy diet full of vegetables and whole grains can help prevent constipation, bloating or excessive gas. Soluble fiber supplements may also help regulate your digestion.
- Practice food safety when cooking at home to avoid unnecessary bacteria that could cause diarrhea or worse. Make sure vegetables are properly washed, meat is cooked to the appropriate temperature, and kitchen counters and cookware are sanitized and free of cross-contamination.
- Quit smoking and limit your alcohol intake. Smoking can make digestive problems worse, and excessive alcohol can lead to cirrhosis or cancers of the stomach, liver, pancreas and colon.